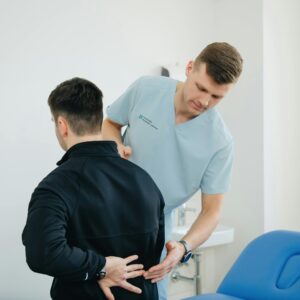
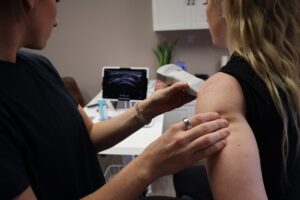
Chronic pain affects nearly eight million Canadians, transforming simple daily activities into exhausting challenges. For residents of Milton, Ontario, where long commutes, physical labor, and active lifestyles are common, persistent pain can disrupt work, family life, and recreational pursuits.
At Tonic Physio, we specialize in comprehensive chronic pain management that addresses both symptoms and underlying causes. This complete guide explores evidence-based approaches to understanding, treating, and living well with chronic pain.
Understanding Chronic Pain
Chronic pain persists beyond normal healing time, typically lasting three months or longer. Unlike acute pain that signals injury or illness, chronic pain often continues after tissues have healed. This persistence occurs because the nervous system itself becomes sensitized, amplifying pain signals and creating self-sustaining pain cycles.
Common chronic pain conditions treated at Tonic Physio include persistent lower back pain, neck and shoulder tension, osteoarthritis, fibromyalgia, neuropathic pain, and chronic headaches. Each condition requires personalized assessment and targeted treatment approaches.
The Biopsychosocial Approach to Pain Management
Modern pain science recognizes that chronic pain involves biological, psychological, and social factors. Effective treatment addresses all three dimensions rather than focusing solely on tissue damage.
Biological Factors
Tissue damage, inflammation, and nervous system changes create the physical experience of pain. Physiotherapy addresses these factors through manual therapy, exercise, and modalities that promote healing and reduce sensitization.
Psychological Factors
Stress, anxiety, depression, and catastrophizing amplify pain perception and create avoidance behaviors that worsen disability. Addressing these factors through education, relaxation techniques, and cognitive strategies improves outcomes significantly.
Social Factors
Work demands, family responsibilities, and social support influence pain experience and recovery. Understanding these contextual factors helps create realistic, sustainable treatment plans that fit your life circumstances.
Physiotherapy for Chronic Pain
Physiotherapy forms the foundation of chronic pain management at Tonic Physio. Our registered physiotherapists use evidence-based techniques to reduce pain, improve function, and prevent recurrence.
Manual Therapy
Hands-on techniques including joint mobilization, soft tissue release, and myofascial therapy reduce muscle tension, improve joint mobility, and decrease pain signaling. These treatments provide immediate relief while creating conditions for healing.
Therapeutic Exercise
Targeted exercise programs build strength, flexibility, and endurance that support the spine and joints. Core stabilization, postural retraining, and graded activity programs restore function progressively without aggravating pain.
Modalities
Advanced treatments including shockwave therapy, electrical stimulation, and ultrasound complement hands-on care. These modalities reduce inflammation, promote tissue repair, and modulate pain signals.
Acupuncture and Dry Needling
Acupuncture provides effective chronic pain relief by modulating the nervous system and promoting natural pain-relief chemistry. Research supports its use for back pain, osteoarthritis, fibromyalgia, and neuropathic pain. Our registered acupuncturists integrate traditional techniques with modern understanding for optimal results.
Dry needling targets myofascial trigger points that contribute to persistent muscle pain. This technique releases tension, improves blood flow, and resets dysfunctional muscle patterns.
Massage Therapy
Registered massage therapy addresses muscle tension, circulation, and stress that exacerbate chronic pain. Our massage therapists specialize in techniques for chronic pain conditions, providing both physical relief and relaxation that supports overall recovery.
Exercise and Movement Strategies
Regular movement is essential for chronic pain management, though many individuals fear exercise will worsen symptoms. Graduated, appropriate activity actually reduces pain over time by improving tissue health, releasing endorphins, and breaking the deconditioning cycle.
At Tonic Physio, we teach active rehabilitation strategies that build confidence and capacity without causing flare-ups. Walking, swimming, yoga, and tai chi offer gentle options for maintaining mobility and fitness.
Self-Management Techniques
Effective chronic pain management extends beyond clinical treatments. Self-management strategies empower you to influence your pain experience daily:
- Pacing activities to avoid overexertion and subsequent crashes
- Stress reduction through breathing exercises, meditation, or mindfulness
- Sleep hygiene to improve restorative rest
- Heat and cold therapy for symptom management
- Ergonomic adjustments at work and home
- Nutrition that supports anti-inflammatory processes
When to Seek Professional Help
While self-management is important, certain situations require professional intervention. Contact Tonic Physio if your pain:
- Persists beyond three months despite self-care efforts
- Significantly limits work, sleep, or daily activities
- Worsens despite treatment attempts
- Causes anxiety, depression, or social withdrawal
- Is accompanied by unexplained weight loss, fever, or neurological symptoms
The Science of Chronic Pain
Understanding chronic pain requires examining how the nervous system processes and maintains pain signals. When tissue damage occurs, nociceptors, specialized nerve endings, detect harmful stimuli and transmit signals through the spinal cord to the brain. The brain interprets these signals as pain, prompting protective responses.
In chronic pain, this system malfunctions. Nerve fibers become hypersensitive, firing in response to harmless stimuli. The spinal cord amplifies signals through wind-up phenomena, where repeated stimulation increases response intensity. The brain’s pain maps expand, creating larger representations of affected areas that perpetuate pain perception.
Central sensitization represents perhaps the most significant mechanism in chronic pain. The central nervous system undergoes neuroplastic changes that lower pain thresholds and increase response duration. Neurons that previously responded only to intense stimuli now react to gentle touch or temperature changes. This sensitization explains why chronic pain often spreads and why previously comfortable activities become painful.
Inflammatory processes also contribute to chronic pain maintenance. While acute inflammation promotes healing, chronic low-grade inflammation perpetuates tissue irritation and nerve sensitization. Cytokines and other inflammatory mediators sensitize nociceptors, creating ongoing pain signals without significant tissue damage.
Types of Chronic Pain
Chronic pain manifests in various forms, each with distinct characteristics and treatment considerations:
Nociceptive Pain
This pain originates from ongoing tissue damage or inflammation. Osteoarthritis, chronic low back pain, and persistent soft tissue injuries produce nociceptive pain. Treatment focuses on reducing tissue irritation while addressing contributing mechanical factors.
Neuropathic Pain
Nerve damage or dysfunction characterizes neuropathic pain. Sciatica, diabetic neuropathy, and post-herpetic neuralgia represent common examples. This pain often feels burning, shooting, or electric and responds to different treatments than nociceptive pain.
Nociplastic Pain
This category describes pain arising from altered nociception without clear tissue damage or nerve injury. Fibromyalgia and irritable bowel syndrome exemplify nociplastic pain. Treatment emphasizes nervous system modulation and central desensitization.
Inflammatory Pain
Autoimmune and inflammatory conditions create pain through persistent immune activation. Rheumatoid arthritis and inflammatory bowel disease represent this category. Managing inflammation while addressing pain provides optimal outcomes.
Psychological Aspects of Chronic Pain
The relationship between pain and psychology is bidirectional. Pain causes emotional distress while psychological factors influence pain experience. Understanding this connection enables comprehensive treatment approaches.
Pain catastrophizing, the tendency to ruminate about pain, magnify its threat, and feel helpless, strongly predicts disability and poor outcomes. Addressing catastrophizing through cognitive-behavioral strategies significantly improves function regardless of pain intensity changes.
Anxiety and depression commonly accompany chronic pain, creating vicious cycles that worsen both conditions. Pain limits activity, reducing enjoyable experiences that normally support mood. Low mood decreases pain tolerance and increases pain perception. Breaking this cycle requires addressing both conditions simultaneously.
Fear-avoidance beliefs, where patients avoid movement due to fear of pain or re-injury, drive deconditioning and disability. Graded exposure to feared activities, guided by physiotherapists, rebuilds confidence and function while demonstrating that movement is safe.
Nutrition and Chronic Pain
Dietary factors influence inflammation, tissue healing, and pain perception. While nutrition alone rarely eliminates chronic pain, appropriate dietary strategies support other treatments.
Anti-inflammatory diets emphasize omega-3 fatty acids from fish and flaxseed, colorful vegetables and fruits rich in antioxidants, nuts and seeds providing magnesium and healthy fats, and spices like turmeric and ginger with proven anti-inflammatory properties.
Protein intake supports tissue repair and muscle maintenance essential for recovery. Adequate hydration maintains tissue elasticity and waste removal. Limiting processed foods, excessive sugar, and trans fats reduces inflammatory burden.
Sleep and Pain
Sleep disturbances and chronic pain frequently coexist, each worsening the other. Pain disrupts sleep through difficulty finding comfortable positions, frequent awakening, and reduced restorative deep sleep stages. Poor sleep increases pain sensitivity, inflammation, and emotional distress.
Addressing sleep hygiene improves both rest and pain. Recommendations include maintaining consistent sleep schedules, creating cool, dark, quiet sleep environments, limiting screens before bedtime, avoiding caffeine after midday, and establishing relaxing pre-sleep routines.
For persistent sleep problems, professional evaluation identifies treatable conditions like sleep apnea or restless leg syndrome that contribute to pain and fatigue.
Workplace Ergonomics
For Milton’s many commuting and desk-working residents, workplace ergonomics significantly impacts chronic pain. Proper workstation setup reduces strain during the eight or more hours spent at work.
Key ergonomic principles include positioning monitors at eye level an arm’s length away, keeping keyboards and mice close to prevent reaching, maintaining feet flat on the floor with hips and knees at ninety degrees, using lumbar support that maintains natural spinal curves, and taking movement breaks every thirty to sixty minutes.
For manual workers, proper lifting techniques, appropriate tool selection, and job rotation reduce repetitive strain. Our WSIB care programs specifically address workplace-related chronic pain.
Long-Term Prognosis
Chronic pain prognosis varies widely based on condition type, duration, contributing factors, and treatment approach. While some chronic pain resolves completely, others require ongoing management. The goal shifts from cure to optimal function and quality of life.
Research demonstrates that multidisciplinary approaches produce the best long-term outcomes. Combining physiotherapy, psychological support, medical management, and self-care strategies addresses all pain dimensions. Patients who actively engage in their care, maintaining exercises and lifestyle modifications, generally achieve superior results.
At Tonic Physio, we emphasize realistic goal setting, celebrating functional improvements even when pain persists. Many patients return to work, recreational activities, and fulfilling social lives despite ongoing symptoms. This functional focus provides hope and motivation throughout the recovery journey.
The Tonic Physio Approach
At Tonic Physio in Milton, we understand that chronic pain is complex and personal. Our approach combines:
- Comprehensive assessment identifying all contributing factors
- Personalized treatment plans addressing your specific needs
- Integration of multiple therapies for comprehensive care
- Education empowering you as an active participant in recovery
- Ongoing support adjusting treatment as your condition evolves
Medication Management in Chronic Pain
While physiotherapy and complementary therapies form the foundation of our approach, medication sometimes plays a supporting role. Understanding medication options helps patients make informed decisions about their care.
Over-the-counter options including acetaminophen and non-steroidal anti-inflammatory drugs provide relief for mild to moderate pain. These medications work best when used strategically rather than continuously. Long-term NSAID use requires medical supervision due to gastrointestinal, cardiovascular, and renal risks.
Prescription medications for chronic pain include muscle relaxants for short-term spasm relief, neuropathic pain agents like gabapentin and pregabalin for nerve-related pain, and topical preparations that deliver medication locally with minimal systemic effects. Our physiotherapists coordinate with physicians to ensure medication supports rather than replaces active rehabilitation.
Opioid medications, while effective for acute pain, generally provide poor outcomes for chronic non-cancer pain. Tolerance, dependence, side effects, and lack of functional improvement make these medications unsuitable for long-term management. Our approach emphasizes active recovery rather than pharmacological masking.
Alternative and Complementary Therapies
Beyond conventional physiotherapy, numerous complementary approaches support chronic pain management. At Tonic Physio, we integrate evidence-based complementary therapies into comprehensive care plans.
Acupuncture demonstrates proven efficacy for several chronic pain conditions. By stimulating specific points, acupuncture modulates nervous system function and promotes natural pain relief mechanisms. Our registered acupuncturists provide this service as part of integrated treatment plans.
Mind-body practices including mindfulness meditation, progressive relaxation, and biofeedback help patients influence their pain experience. These techniques reduce stress responses that amplify pain while improving coping capacity. Even brief daily practice produces measurable benefits.
Yoga and tai chi combine movement, breathing, and mindfulness in formats appropriate for chronic pain patients. These gentle practices improve flexibility, strength, balance, and stress management simultaneously. Our physiotherapists can recommend appropriate styles and modifications.
The Role of Support Systems
Social support significantly influences chronic pain outcomes. Understanding family dynamics, workplace accommodations, and community resources enhances recovery.
Family members often struggle to understand invisible pain conditions. Education helps loved ones provide appropriate support without enabling disability. Open communication about needs, limitations, and goals prevents misunderstanding and resentment.
Workplace accommodations may include modified duties, flexible schedules, ergonomic adjustments, or gradual return-to-work programs. The Workplace Safety and Insurance Board provides support for work-related conditions, while human rights legislation protects employees with disabilities.
Support groups connect individuals experiencing similar challenges. Sharing experiences, coping strategies, and encouragement reduces isolation that often accompanies chronic pain. Both in-person and online communities provide valuable peer support.
Preventing Chronic Pain Development
While this guide focuses on managing existing chronic pain, prevention deserves attention. Many chronic pain conditions develop from untreated acute injuries or persistent poor mechanics.
Early, appropriate treatment of acute injuries prevents the nervous system changes that lead to chronicity. Complete rehabilitation before returning to full activity, rather than stopping when pain subsides, ensures tissues heal properly and movement patterns normalize.
Addressing biomechanical issues before they cause symptoms prevents many overuse conditions. Postural correction, movement retraining, and appropriate conditioning reduce cumulative strain that eventually produces pain.
Stress management prevents tension-related pain from becoming chronic. Regular relaxation practice, healthy boundaries, and adequate sleep support resilience against pain development.
Living Well with Chronic Pain
Chronic pain does not have to define your life. With appropriate treatment, self-management, and support, many individuals return to meaningful activities and improved quality of life. The journey requires patience and persistence, but progress is possible.
Success Stories from Milton Residents
While every patient’s journey is unique, common themes emerge among those who successfully manage chronic pain. Understanding these patterns provides hope and guidance for others beginning their recovery.
Successful patients typically embrace active participation in their care rather than seeking passive fixes. They attend appointments consistently, perform home exercises diligently, and implement lifestyle modifications recommended by their team. This engagement transforms treatment from something done to them into something done with them.
Patience characterizes those who achieve lasting improvement. Chronic pain develops over time and requires time to change. Expecting immediate resolution leads to disappointment and abandonment of effective treatments before benefits manifest. Most patients notice meaningful changes within eight to twelve weeks of consistent care.
Flexibility helps patients navigate the ups and downs of chronic pain management. Flare-ups occur despite best efforts. Successful patients view these setbacks as temporary rather than catastrophic, adjusting activities while maintaining core self-care practices.
Goal orientation keeps patients motivated through difficult periods. Setting functional objectives like walking duration, work hours, or recreational participation provides concrete measures of progress. Celebrating achievements, however modest, builds confidence and momentum.
Research and Innovation in Chronic Pain
Pain science continues evolving, offering new hope for chronic pain sufferers. Emerging research areas include neuroplasticity-based therapies that retrain the nervous system, virtual reality interventions that modulate pain perception, genetic testing that predicts treatment response, and personalized medicine approaches that match interventions to individual characteristics.
At Tonic Physio, we stay current with evidence-based innovations, integrating promising approaches into our practice when research supports their effectiveness. Our commitment to continuing education ensures patients benefit from the latest advances in pain management.
If you are struggling with chronic pain in Milton, contact Tonic Physio today. Our experienced team will assess your condition, explain your options, and partner with you in developing a comprehensive management plan that addresses your unique situation and goals.